FOR DOCTORS – PART IV
Grade II or Distal Hypospadias: “The Slit-like adjusted Mathieu (SLAM) Technique”
The meatal-based flap technique of Mathieu is the most popular technique for distal hypospadias repair and has withstood the test of time. However, the major drawback of the original Mathieu technique is the final appearance of the meatus (a smiling meatus that is not very terminal). The Slit-like adjusted Mathieu (SLAM) helps to employ the Mathieu operation in all forms of distal hypospadias and gives a terminal, slit like meatus. This will include about 70 to 80 % of patients with hypospadias. The only contraindication is the presence of severe chordee distal to the hypospadiac meatus (very rare in distal hypospadias).
Operative steps:
- The boundaries of the urethral plate are outlined. A U-shaped incision is outlined. The two parallel incisions at the glans region start along the true mucosal urethral plate to have large, wide glanular wings. At the distal end, the two incision converge as shown to have a slit-like meatus and to avoid having sutures at the meatus. The two lateral incisions diverge near the meatus to produce a wide flap.
- Fig 1b.: Flap mobilisation: Using a sharp scissors, the incision is deepened starting near the coronal sulcus, the lateral skin edge (not the flap) is held with fine toothed forceps and fascia and corpus spongiosum are included with the flap as much as possible.
- Fig 1c.: Angle epithelium excision: The epithelium at the proximal two angles of the flap is excised maintaining the fascia.
- Fig.1d: Urethroplasty: The edges of the flap are fixed to the converging edges of the urethral plate 2-3 mm from the distal end of the incision. Urethroplasty is carried out using 6/0 vicryl on a sharp needle in a continuous subcuticular fashion starting 3 mm proximal to the angle of the flap. A sealing second suture line in a continuous fashion is carried out.
- Fig. 1e:. V-Excision: A triangle is removed from the tip of the flap to help having a slit like meatus.
- Fig 1f, g: Glans and skin closure: The glanular wings are approximated around the new urethra and the penile skin is closed. Notice that the new meatus has one stitch only at 6 O’clock.
Complications: Fistula occurs in 2 – 5 % of patients.
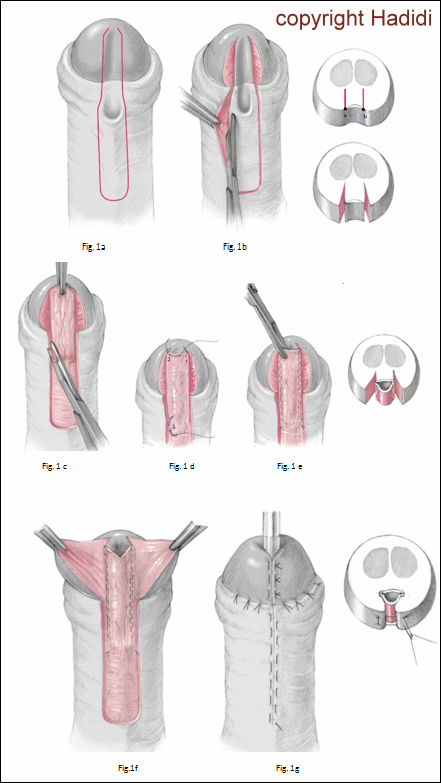
Fig. 9: The SLAM technique for distal hypospadias
Grade IIIa – Proximal hypospadias: “Lateral Based Onlay (LABO) Flap”
The lateral Based Onlay (LABO) flap may be used in proximal hypospadias without deep chordee that requires division of the urethral plate to straighten the penis. It is of particular value in patients with small glans. The principle is to use the lateral penile skin as well as part of the prepuce to reconstruct the new urethra. It has the advantages over the classic lateral based flap of less complications, only one catheter through the penis for one week and less hospital stay (8 days after surgery).
Operative steps:
- A U-shaped incision is outlined. The two parallel incisions go very deep into the glans and converge as shown to have a slit-like meatus. The left incision stops at the coronal sulcus and continues distally in the prepuce at the muco-cutaneous junction and constitutes the medial border of the LABO flap. The flap is designed to have a wide base as shown in the figure.
- Fig 2b.: Flap mobilisation: The right incision is deepened starting near the coronal sulcus.
- Apex suture: The tip of the medial border of the LABO flap (A) is sutured to the urethral plate 2 mm proximal to the edge (A´).
- Fig.2c.: Urethroplasty: The medial border of the LABO flap is sutured to the left edge of the urethral plate.
- Fig.2d: The LABO flap is turned over the catheter.
- Fig.2e: The second apex stitch is fixed 2 mm from the tip of the urethral plate incision.
- Fig.2f: Urethroplasty is completed on the right side. A triangle is removed from the tip of the flap to help having a slit like meatus.
- Fig 2g: A second intermediate layer is used from the scrotal dartos/tuncia vagnialis.
- Fig 2h: Glans and skin closure: The glanular wings are approximated around the new urethra and the penile skin is closed. Notice that the new meatus has one stitch only at 6 O’clock.
Complications: 5-7 % in the form of fistula, glans dehiscence or skin prolapsed from the meatus.
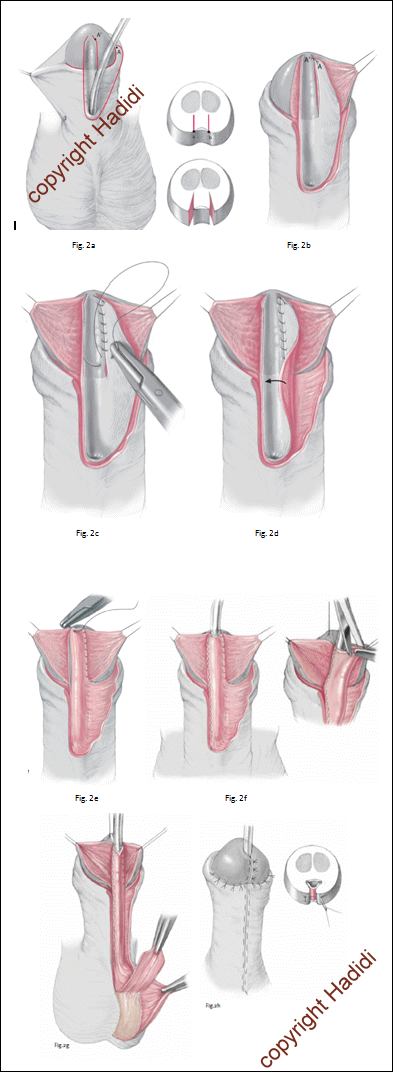
Fig 10: The lateral based Onlay (LABO) technique for proximal hypospadias
Grade IIIb – Proximal hypospadias with deep chordee: “Lateral Based Flap”
The lateral based flap may be used in all types of proximal hypospadias This flap with double blood supply, combines the advantages of meatal-based flap, and preputial pedicle flap techniques into one procedure without the need for an intervening anastomosis. It also allows for extensive excision of ventral chordee and the urethral plate (if necessary) without damaging the flap.
Operative steps:
- A deep Y-shaped incision is made on the glans. The centre of the Y is where the tip of the neo-meatus will be located. The upper two short limbs of the Y are 0.5 cm long. The long vertical limb Y extends down the whole length of the glans penis to the coronary sulcus (Fig. 9 a). The resultant three flaps are elevated and a core of soft tissue is excised to create a space for the neo-urethra (Fig. 9 b).
- Meticulous excision of any chordee or fibrous bands is carried out. This fibrous tissue is particularly heavy in the midline but may extend well laterally. The meatus is assessed and a cut back is made to widen the meatus (Fig. 9 c).
- A rectangular skin strip is outlined extending proximally from the urethral meatus staying in the midline in the scrotum to avoid potentially hair bearing skin. The skin strip is extended distally and laterally by curving towards the prepuce. This allows for formation of a very long tube that can reach the tip of the glans wherever the original position of hypospadias meatus is (Fig. 9 d).
- The skin incision is carried completely around the meatus leaving a small cuff of skin. The meatus is freed proximally. The adjacent penile skin is elevated (rather than the flap). The flap with its pedicle is mobilised through the dorsum of the penis and down to the root of the penis to avoid penile rotation.
- The skin strip and proximal cuff are tubularised around a Nelaton catheter size 10 Fr inside the urethra. The author prefers to use Vicryl 6/0 on a cutting needle. Suturing is carried out from distal to proximal in a subcuticular continuous manner. Several reinforcing interrupted stitches are usually taken to form water tight tube (Fig. 9 e).
- The neomeatus is then constructed by suturing the terminal end of the neourethra to the central V of the glans. A final slit like meatus is obtained by excising a small V from the tip of the neo-urethra. Then, the glanular wings are wrapped around the neourethra and approximated in the midline. When completed a near normal wide meatus is created at the tip of a conical shaped glans. The long anastomotic contact between the neo-meatus and glans created by the Y glanuloplasty is important to create a wide meatus and avoid post operative meatal stenosis. The vascular areolar subcutaneous tissue layer is then used to provide a complete covering for the neourethra (Fig. 9 f). The skin is closed in the midline using 6/0 Vicryl in a continuous transverse mattress. This helps to simulate the normal ventral median skin raphae (Fig. 9 g). A percutaneous suprapubic cystocath is inserted into the bladder for 10 – 14 days. A compression dressing is applied for 6 hours for haemostasis.
Complications: Fistula occurs in 6 – 12 % of patients. Penile rotation may occur if the pedicle is not mobilized down to the root of the penis.
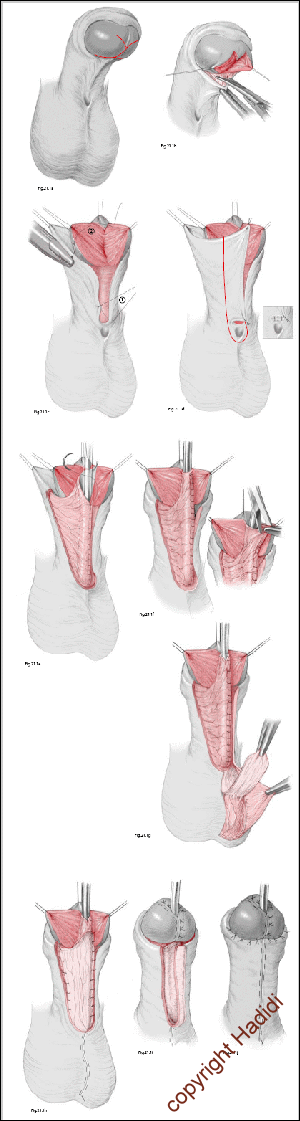
Fig. 11: Steps of lateral-based (LB) flap technique for single stage repair of proximal hypospadias. (a, b) Y-shaped deep incision of the glans; (c) chordectomy; (d) outline skin incision and flap mobilisation; (e) formation of the neourethra; (f) glanulomeatoplasty; (g) protective intermediate layer; (h) skin closure