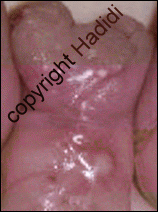
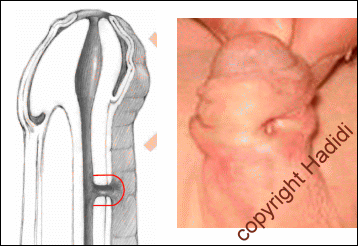
About one third of patients referred to the Hypospadias Centre had a failed TIP procedure. The concept of the TIP procedure results in leaving a large raw surface in the reconstructed urethra. This raw surface usually contracts during healing resulting in a very narrow urethra and persistent fistula. Occasionally, the whole wound disrupts completely and urine comes out from the original opening. The condition becomes more complicated when the surgeon during the TIP procedure has excised the forskin. This makes the job of correction more difficult as there is no excess skin available to reconstruct the narrow urethra.
About one third of patients referred to the Hypospadias Centre had a failed TIP procedure. The concept of the TIP procedure results in leaving a large raw surface in the reconstructed urethra. This raw surface usually contracts during healing resulting in a very narrow urethra and persistent fistula. Occasionally, the whole wound disrupts completely and urine comes out from the original opening. The condition becomes more complicated when the surgeon during the TIP procedure has excised the forskin. This makes the job of correction more difficult as there is no excess skin available to reconstruct the narrow urethra.
A report from Anonymous Patient:
My Life With Hypospadias
The congenital malformation of the urethra is usually surgically corrected in early childhood. I am 28 years old now and I have not undergone this correction. It was not until puberty that I noticed that my penis actually looks slightly different from the other boys’ when the foreskin is retracted. Over time I felt ashamed, afraid of being exposed and did not want to stand in a row next to the others at the urinal. To avoid this I tried to go to the toilet alone or chose the cabin. To be made fun of for sitting down on a toilet while urinating was less annoying than a possible discovery of hypospadias, which caused me constant anxiety. Especially in puberty you don’t want to be “different”. I tried to suppress the malformation and avoided any sexual advances and contacts. It would certainly have been better if I had turned to my parents with this burden, but I was even ashamed to talk to them and did not bring the subject up to them. The repression eventually became part of my every day life, subconsciously rather than self-protecting, because the panic and feeling of being different did affect my psyche.
It was only at the age of 20 that I learned by chance via the Internet that my congenital malformation of the urethra was a so-called hypospadias and that it occurs relatively frequently in newborn boys. The information on surgical corrections was mainly related to infants. Here it was always emphasized that an operation at the age between 12 and 18 months was the most advantageous. I assumed that a successful operative correction in adulthood was not a safe option due to the higher complication rate. I therefore rejected this option for the time being. Nevertheless, I felt better when I realized that I was not the only one who has this congenital malformation and that surgery was basically possible. From this point on, I felt a little safer with hypospadias and dared to allow physical contact. The women I met reacted very differently to hypospadias. I experienced rejection, indifference but also understanding. Nevertheless, getting to know each other is relatively difficult, as the malformation continues to be very unpleasant for me and for this reason I try to find out in advance how this person would react to such malformations. Of course, this does not always work as hoped and oven seems contrived and awkward. A normal, relaxed getting to know each other is not possible for me.
The urethral malformation does not restrict me very much from a purely functional point of view, rather it represents a great psychological strain. Over time it becomes more and more difficult for me to live with it without having worries about it and I do suffer from it. I want a change and so I resumed the research on the topic of hypospadias corrections for adults and came across the website of the hypospadias centre of the Emma Klinik in Seligenstadt. The treatment spectrum on the main page already lists the surgical correction for adults. I arranged an appointment with Prof. Hadidi. Among other things, Prof. Hadidi explained to me straightforwardly and plausibly the possible risks of a surgical correction and seemed very professional to me. Especially the specialization in hypospadias as well as Prof. Hadidi’s expertise in adults and the his international reach have convinced me. I am now awaiting the operation and hope that everything will go well.
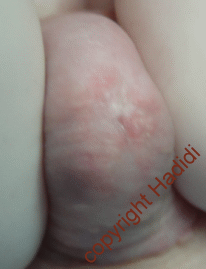 |
 |
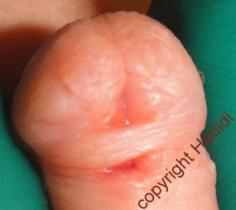
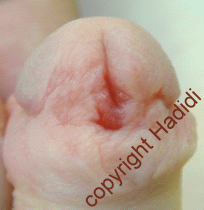
| Pin point meatus after TIP | more urine from fistula |
 |
 |

 We tell the parents not to look at the penis for one month after surgery until the swelling disappear and the wound has healed by 70%.
We tell the parents not to look at the penis for one month after surgery until the swelling disappear and the wound has healed by 70%.