FOR DOCTORS – PART VI
Two Stage repair
A small group of patients with severe proximal hypospadias, chordee, and a small phallus as well as patients with recurrent hypospadias and fibrous unhealthy skin may benefit from a two-stage procedure (Fig. 10).
In the first stage, a circumferential incision is made proximal to the coronal sulcus, the chordee is excised, and the penile shaft is de-golved. Penile straightening and removal of all chordee tissue must be confirmed by the use of the artificial erection test.
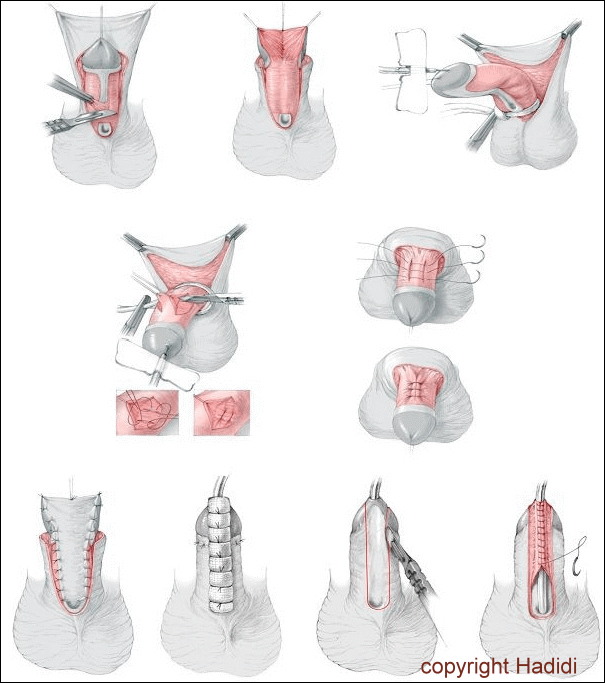
Fig. 12: Steps of two stage repair: identification of chordee, excision of ventral chordee and plication if needed. Coverage of raw surface with skin graft. Tubularisation in the second operation.
The glans is divided deeply in the midline to the tip. The dorsal foreskin is unfolded carefully and divided in the midline. A midline closure is performed, and the midline sutures catch a small portion of Buck’s fascia. The bladder is drained with an 8 French Silastic Foley catheter for approximately 5 to 7 days.
If there is inadequate genital skin available, buccal mucosa or rarely bladder mucosa may be used. The buccal mucosa is harvested from the inner surface of the cheek or the inner surface of the upper or lower lip. The parotid duct is identified opposite the upper molars, and cannulated with 3-0 nylon. The graft is outlined and the submucosa infiltrated with 1% lignocaine containing 1:2000 epinephrine. The graft is incised and the mucosa is dissected away by sharp dissection.
The second stage of the procedure is carried out 6 to 12 months later. The previously transferred skin or mucosa is used to reconstruct the glans and urethra. A 16-mm diameter strip is measured, extending to the tip of the glans. The strip is tubularized with a running subcuticular stitch of 6-0 Vicryl® all the way to the tip of the glans. Tension is reduced by generous mobilization and undermining of adjacent tissues. A protective intermediate layer (either tunica vaginalis or dartos) helps to reduce post-operative complications.
The lateral skin edges are mobilized, and the remaining tissue is closed over the repair in at least two layers. A strip of skin (3 – 5 mm wide) is de-epithelialised on one side to provide a raw surface of deep dermis. This is achieved by cutting 2 or 3 fine longitudinal strips with a pair of small curved-on-scissors. The medial edge of the shaved flap is brought across the buried urethroplasty and sutured to fascial tissue beneath the other flap (double breasting).
Artificial erection test and chordee (curvature) correction
Ventral curvature (chordee) may be evaluated by the artificial erection test. There are two types of chordee associated with hypospadias:
- Chordee associated with distal hypospadias (skin chordee). This superficial chordee is subcutaneous, proximal to the meatus and can be corrected by mobilization of the skin proximal to the meatus.
- The other type of chordee is commonly associated with proximal hypospadias. It is usually deep, fibrous and located distal to the meatus. This curvature may be corrected either by Heineke Mikulicz technique, dorsal placation, corporal rotation or the “Split & Roll technique”.
Use of protective intermediate layer
The use of an intermediate or interposition layer between the neourethra and the skin layer has greatly improved the results following hypospadias surgery and reduced complications. Types of protective intermediate layer include:
- Durham Smith (1973) de-epithelialization
- Snow (1986) described the use of Tunica vaginalis wrap.
- Retik (1988) was the first to use dorsal subcutaneous flap from the prepuce.
- Motiwala (1993) described the use of Dartos flap from the scrotum.
- Yamataka (1998) reported the use of external spermatic fascia flap
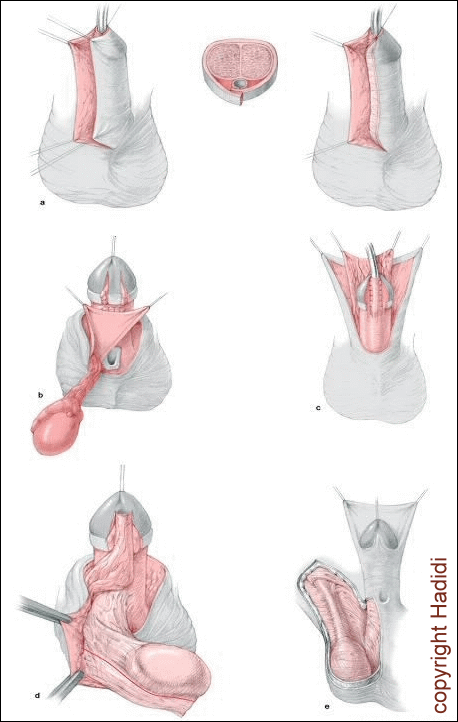
Some technical points:
- Stenting: several studies showed that stenting of the neourethra may be associated with more complications.
- Dressing: several studies also showed that the type of dressing has a major impact on the outcome of surgery, some studies showed better results without any dressing at all.
- In general: if a complication occurs, one should not operate again before 6 months to allow time for complete healing of the tissues and to give better chance for the success of surgery.
- Fistula management: The most important two steps in the management of fistula are to exclude distal obstruction and to excise the cornu of the fistula to reduce the chances of recurrence.
- Failed distal hypospadias repair: the technique to be adopted depends on the degree of fibrosis and the amount of healthy tissue available. Failed Mathieu repair does not necessarily mean that we can not do another Mathieu repair.
- Failed proximal hypospadias repair: the most important step is to excise all the unhealthy tissues. Then, according to the healthy tissues available, one may use lateral based flap, a graft … etc.
- If scrotal transposition is present, it is suggested to correct hypospadias first and then correct the scrotal transposition at a later stage to ensure adequate blood supply to the flap used in urethroplasty.
- The role of tissue culture and tissue engineering is a point of major research. So far the indications for tissue culture in the field of hypospadias are still limited.


